
By the age of 18, the average adult has 32 teeth; 16 teeth on the top and 16 teeth on the bottom. Each tooth in the mouth has a specific name and function. The teeth in the front of the mouth (incisors, canine, and bicuspid teeth) are ideal for grasping and biting food into smaller pieces. The back teeth (molar teeth) are used to grind food up into a consistency suitable for swallowing.
The average mouth is made to hold only 28 teeth. It can be painful when 32 teeth try to fit in a mouth that holds only 28 teeth. These four other teeth are your third molars, also known as "wisdom teeth."
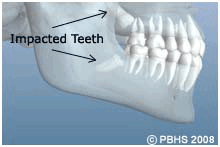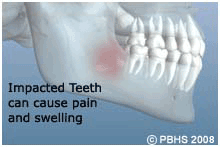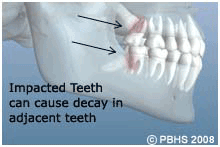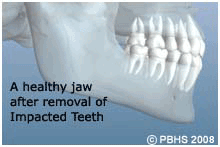
Wisdom teeth are the last teeth to erupt within the mouth somewhere between ages 12-30 years. Rarely do they align properly and the gum tissue is healthy so, wisdom teeth do usually have to be removed. The extraction of wisdom teeth is necessary when they are prevented from properly erupting within the mouth. They may grow sideways, partially emerge from the gum, and even remain trapped beneath the gum and bone. Impacted teeth can take many positions in the bone as they attempt to find a pathway that will allow them to successfully erupt.
These poorly positioned impacted teeth can cause many problems. When they are partially erupted, the opening around the teeth allows bacteria to grow and will eventually cause an infection. The result: swelling, stiffness, pain, and illness. The pressure from the erupting wisdom teeth may move other teeth and disrupt the orthodontic or natural alignment of teeth. The most serious problem occurs when tumors or cysts form around the impacted wisdom teeth, resulting in the destruction of the jawbone and healthy teeth. These teeth are generally soft, chalky and poorly developed and prone to decay which can spread to the adjacent teeth. Removal of the offending impacted teeth usually resolves these problems. Early removal is recommended to avoid such future problems and to decrease the surgical risk involved with the procedure.
With an oral examination and x-rays of the mouth, Dr. Teenier can evaluate the position of the wisdom teeth and predict if there are present or may be future problems. Studies have shown that early evaluation and treatment result in a superior outcome for the patient. Patients are generally first evaluated in the mid-teenage years by their dentist, orthodontist or by an Oral and Maxillofacial Surgeon. Removal prior to full root development and infection can prevent complications.
All outpatient surgery is performed under appropriate anesthesia to maximize patient comfort. Dr. Teenier has the training, license and experience to provide various types of anesthesia for patients to select the best alternative.
In most cases, the removal of wisdom teeth is performed under local anesthesia, with the addition of laughing gas (nitrous oxide/oxygen analgesia), IV sedation or general anesthesia. These options, as well as the surgical risks (i.e., sensory nerve damage, sinus complications), will be discussed with you before the procedure is performed. Once the teeth are removed, the gum is sutured. To help control bleeding, bite down on the gauze placed in your mouth. You will rest under our supervision in the office until you are ready to be taken home. Upon discharge, your postoperative kit will include postoperative instructions, gauze, teabags, a prescription for pain medication, antibiotics, and a follow-up appointment. If you have any questions, please do not hesitate to call us at 361-814-3223.
Our services are provided in an environment of optimum safety that utilizes modern monitoring equipment and staff who are experienced in modern anesthesia techniques.
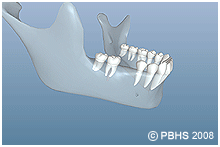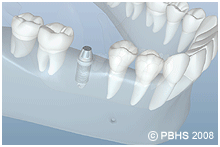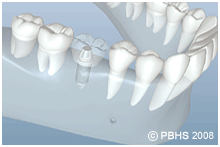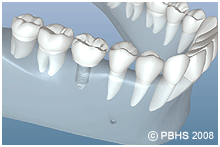
Dental implants (man-made tooth roots) are changing the way people live. They are designed to provide a foundation for replacement teeth that look, feel, and function like natural teeth. The person who has lost teeth regains the ability to eat virtually anything, knowing that teeth appear natural and that facial contours will be preserved. Patients with dental implants can smile with confidence.
The implants themselves are tiny titanium posts/man-made tooth roots that are surgically placed into the jawbone where teeth are missing. These metal anchors act as a man made tooth root substitutes. The bone bonds with the titanium, creating a strong foundation for artificial teeth. Small posts that protrude through the gums are then attached to the implant. These posts provide stable anchors for artificial replacement teeth. The physiology is similar to healing of a total knee or hip joint.
Implants also help preserve facial structure, preventing bone deterioration that occurs when teeth are missing, which can change an aged appearance to the face.
For most patients, the placement of dental implants involves two surgical procedures. First, the planning phase/discussion of implants should begin prior to extraction or removal of the broken or non-viable teeth. Second, implants are placed within your jawbone. For the first three to six months following surgery, the implants heal beneath the surface of the gums where the implant prosthetics gradually bonds with the jawbone. In many cases you can wear temporary dentures and eat a soft diet during this time. At the same time, your restorative dentist/dental specialist is forming new replacement teeth.
After the implant has bonded to the jawbone, the second phase begins. Dr. Teenier will uncover the implants and attach small posts that protrude through the gums and will act as anchors for the artificial teeth. When the artificial teeth are placed, these posts will not be seen. The entire procedure usually takes four to eight months. Most patients experience minimal disruption in their daily life.
Using the most recent advances in dental implant technology, in some specific cases, Dr. Teenier is able to place single stage implants. The implant and temporary tooth are placed at the same time. These implants do not require a second procedure to uncover them, but do require a minimum of four to six weeks of healing time before permanent artificial teeth are placed. There are even situations where the implants can be placed at the same time as a tooth extraction – further minimizing the number of surgical procedures. Discuss these possibilities with Dr. Teenier.
Dental Implant placement is a team effort between an Oral and Maxillofacial Surgeon and a restorative dentist and or dental specialist. Dr. Teenier performs the actual implant surgery, initial tooth extractions, and bone grafting if necessary. The restorative dentist (your dentist) or dental specialist fits and makes the temporary/permanent prosthesis/teeth/dentures. Your dentist will also make any temporary prosthesis needed during the implant process. We also utilize platelet rich plasma (PRP) technology which aide in the healing of the bone to implant and healing of the wound. This process concentrates your own growth and healing factors to aid in more predictable healing. It is of the utmost importance that a team approach is utilized and much planning goes into every case. Seldom is it beneficial to have one doctor attempt to be “master” of all procedures.
A single tooth replacement (crown) is used to replace one missing tooth – each prosthetic tooth attaches to its own implant. A bridge can replace two or more teeth and may require two or more implants. Complete dentures can be placed to replace all the teeth in your upper or lower jaw and covered to the implants. The number of implants varies depending upon which type of prosthesis is needed and recommended by the restoring doctor and Dr. Teenier during the planning stage as well as how much bone is present for the implants.
Dr Teenier performs in-office implant surgery in a hospital-style operating suite in his office, thus optimizing the level of sterility. Seldom is inpatient hospital implant surgery needed for patients who have special medical or anesthetic needs or for those who need extensive bone grafting from the jaw, hip, skull, leg, rib, etc.
Once you learn about dental implants, you finally realize there is a way to improve your quality of life. When you lose several teeth – whether it’s a new situation or something you have lived with for years – chances are you have never become fully accustomed to losing such a vital part of yourself, and speech and eating are negatively affected. Dental implants can be your doorway to renewed self confidence and peace of mind. Think of dental implants as an improvement of quality of life and self esteem versus going to the dentist for regular treatment.
Each case needs a physical exam and collaboration with the restorative dentist/dental specialist prior to surgery for best results. Our goal is to maximize the success of your treatment. It is similar to building a home. Different contraltos do different procedures, but no one person can do everything as well as a group of individuals thinking and working together.
Dental implants can be your doorway to renewed self-confidence and peace of mind.
A Swedish scientist and orthopedic surgeon, Dr. Per-Ingvar Branemark, developed this concept for oral rehabilitation more than 35 years ago. With his pioneering research, Dr. Branemark opened the door to a lifetime of renewed comfort and self-confidence for millions of individuals facing the frustration and embarrassment of tooth loss. Think of implants as the same technology as replacing any other joint by an orthopedic surgeon just done in a different fashion but within the mouth and face.
Many times traditional dental treatment is appropriate, however why sacrifice/cut down the structure of surrounding good teeth to bridge a space? In addition, removing a denture or a “partial” at night may be inconvenient, not to mention that dentures that slip can be uncomfortable and rather embarrassing while eating and talking. Sometimes removing perfectly good crowns to replace a missing tooth with a bridge may also cause those teeth to act up and result in additional treatment and cost.
If you are considering implants, your mouth must be examined thoroughly and your medical and dental history reviewed. If you mouth is not ideal for implants it usually involves lack of width of the jaw, ways of improving outcome, such as bone grafting, may be recommended. Sometimes the best restoration is routine dental bridges, crowns or dentures. By allowing the doctor to consult with you, conduct an exam with radiographs, he will be able to tell you what is most appropriate.
The majority of dental implants and bone graft can be performed in the office under local anesthesia, with sedation or general anesthesia. Patient preference and the length and case type will determine this generally. Implant cases can range from very straightforward to complex and may require multiple meetings with the restorative dentist/dental specialist and Oral Maxillofacial Surgeon.
Once the implants are in place, they will serve you well for many years if you take care of them and keep your mouth healthy. This means taking the time for good oral hygiene (brushing and flossing) and keeping regular appointments with your dental specialists for cleaning and inspection.
The short answer is “It depends.” Bridges and crowns will need replacement due to breakdown of underlying tissue and wear. Implants if properly cared for, should last a long time. So the cost comparison is important and should be considered but in most cases they are equivalent.
Placing a dental implant requires a number of steps, generally involving several professionals. Much like building a house, seldom is one person master of all trades and when it comes to implants with the team approach you get the best of all worlds at no additional costs.
Every case is different even on the basic steps needs, so costs vary. A consultation with medical history and some basic imaging is necessary to predict success and cost.
While Bridges and Dentures can be less expensive at the outset, you should consider these options have some considerable continuing expenses. Bridges, by their structure, cut down the neighboring abutment teeth - which can lead to weakness and repeated treatments such as root canal therapy and/or cracked/fractured teeth. Dentures cannot preserve the jaw bone the way Dental Implants can, so the jaw shrinks as the bone is resorbed, leading to ill-fitting Dentures and repeated rounds of re-fitting and re-placing these prostheses. Over a lifetime, Dental Implants can be the most cost-effective as well as the best functional and esthetic choice. Dr. Teenier will have a frank discussion with you to decide if you are an implant candidate or not. Sometimes bridge, crown or dentures are just fine.
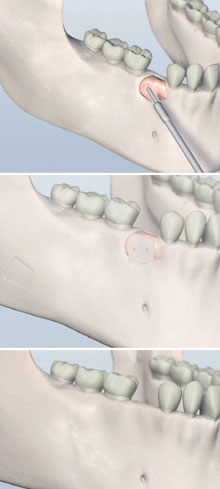
Bone grafting can be needed for many reasons in the facial region. Congenital defects (being born & bone in ages shrinks). Over a period of time, the jawbone associated with missing teeth atrophies or is reabsorbed. This often leaves a condition in which there is poor quality and quantity of bone suitable for placement of dental implants. In some situations, patients are not candidates for placement of dental implants.
Today, we have the ability to grow bone or transplant where needed. This not only gives us the opportunity to place implants of proper length and width, it also gives us a chance to restore functionality and aesthetic appearance.
Bone grafting can repair implant sites with inadequate bone structure due to previous extractions, gum disease or injuries. The bone is either obtained from a tissue bank or your own bone is taken from the jaw, hip or tibia (below the knee). Sinus bone grafts can also be performed to replace bone in the posterior upper jaw or skull. Special membranes may be utilized that dissolve under the gum and protect the bone graft and encourage bone regeneration. This is called guided bone regeneration or guided tissue regeneration.
Major bone grafts are typically performed to repair larger bone defects of the jaws. These defects may arise as a result of traumatic injuries, tumor surgery, or congenital defects. Large defects are repaired using the patient’s own bone. This bone is harvested from a number of different sites depending on the size of the defect. The skull (cranium), hip (iliac crest), and lateral knee (tibia), are common donor sites. These procedures are routinely performed in an operating room and require a short hospital stay.
The maxillary sinuses are behind your cheeks and on top of the upper teeth. Sinuses are like empty rooms that have nothing in them. Some of the roots of the natural upper teeth extend up into the maxillary sinuses. When these upper teeth are removed, there is often just a thin wall of bone separating the maxillary sinus and the mouth. Dental implants need bone to hold them in place. When the sinus wall is very thin, it is impossible to place dental implants in this bone.
There is a solution and it’s called a sinus graft or sinus lift graft. The dental implant surgeon enters the sinus from where the upper teeth used to be. The sinus membrane is then lifted upward and donor bone is inserted into the floor of the sinus. Keep in mind that the floor of the sinus is the roof of the upper jaw. After several months of healing, the bone becomes part of the patient’s jaw and dental implants can be inserted and stabilized in this new sinus bone.
The sinus graft makes it possible for many patients to have dental implants when years ago there was no other option other than wearing loose dentures.
If enough bone between the upper jaw ridge and the bottom of the sinus is available to stabilize the implant well, sinus augmentations and implant placement can sometimes be performed as a single procedure. If not enough bone is available, the sinus augmentation will have to be performed first, then the graft will have to mature for several months, depending upon the type of graft material used. Once the graft has matured, the implants can be placed.
In severe cases, the ridge has been reabsorbed and a bone graft is placed to increase ridge height and/or width. This is a technique used to restore the lost bone dimension when the jaw ridge gets too thin to place conventional implants. In this procedure, the bony ridge of the jaw is literally expanded by mechanical means. Bone graft material can be placed and matured for a few months before placing the implant.
An impacted tooth simply means that it is “stuck” and cannot erupt into function. Patients frequently develop problems with impacted third molar (wisdom) teeth. These teeth get “stuck” in the back of the jaw and can develop painful infections among a host of other problems (see Impacted Wisdom Teeth under Procedures). Since there is rarely a functional need for wisdom teeth, they are usually extracted if they develop problems. The maxillary (upper mandible) cuspid (upper eyetooth) is the second most common tooth to become impacted. The cuspid tooth is a critical tooth in the dental arch and plays an important role in your “bite”. The cuspid teeth are very strong biting teeth and have the longest roots of any human teeth. They are designed to be the first teeth that touch when your jaws close together so they guide the rest of the teeth into the proper bite.
Normally, the maxillary/mandibular cuspid teeth are the last of the “front” teeth to erupt into place. They begin development at 6-9 years and usually come into place around age 13 and cause any space left between the upper front teeth to close tighter together. If a cuspid tooth gets impacted (stuck), every effort is made to get it to erupt into its proper position in the dental arch prior to complete root formation. The techniques involved to aid eruption can be applied to any impacted tooth in the upper or lower jaw, but most commonly they are applied to the maxillary cuspid (upper eye) teeth. Sixty percent of these impacted eyeteeth are located on the palatal (roof of the mouth) side of the dental arch. The remaining impacted eye teeth are found in the middle of the supporting bone but stuck in an elevated position above the roots of the adjacent teeth or out to the facial side of the dental arch. Dr. Teenier will examine you and give you an idea of the placement of your impacted canines.
The older the patient, the more likely an impacted eyetooth will not erupt by nature’s forces alone even if the space is available for the tooth to fit in the dental arch. The American Association of Orthodontists recommends that a panorex screening x-ray, along with a dental examination, be performed on all dental patients at around the age of seven years to count the teeth and determine if there are problems with eruption of the adult teeth. It is important to determine whether all the adult teeth are present or are some adult teeth missing. Are there extra teeth present or unusual growths that are blocking the eruption of the eyetooth? Is there extreme crowding or too little space available causing an eruption problem with the eyetooth? This exam is usually performed by your general dentist or hygienist who will refer you to an orthodontist if a problem is identified. Treating such a problem may involve an orthodontist placing braces to open spaces to allow for proper eruption of the adult teeth. Treatment may also require referral to an oral surgeon for extraction of over-retained baby teeth and/or selected adult teeth that are blocking the eruption of the all-important eyeteeth. The oral surgeon will also need to remove any extra teeth (supernumerary teeth) or growths that are blocking eruption of any of the adult teeth. If the eruption path is cleared and the space is opened up by age 11-12, there is a good chance the impacted eyetooth will erupt with nature’s help alone. If the eyetooth is allowed to develop too much (age 13-14), the impacted eyetooth may not erupt by itself even with the space cleared for its eruption. If the patient is too old (over 20), there is a much higher chance the tooth will be fused in position. In these cases the tooth will not budge despite all the efforts of the orthodontist and oral surgeon to erupt it into place. Sadly, the only option at this point is to extract the impacted tooth and consider an alternate treatment to replace it in the dental arch (crown on a dental implant or a fixed bridge).
In cases where the eyeteeth will not erupt spontaneously, the orthodontist and oral surgeon work together to get these unerupted eyeteeth to erupt. Each case must be evaluated on an individual basis but treatment will usually involve a combined effort between the orthodontist and the oral surgeon. The most common scenario will call for the orthodontist to place braces on the teeth (at least the upper arch). A space will be opened to provide room for the impacted tooth to be moved into its proper position in the dental arch. If the baby eyetooth has not fallen out already, it is usually left in place until the space for the adult eyetooth is ready. Once the space is ready, the orthodontist will refer the patient to the oral surgeon to have the impacted eyetooth exposed, bracketed and chain placed.
In a simple surgical procedure performed in the surgeon’s office, the gum on top of the impacted tooth will be lifted up to expose the hidden tooth underneath. If there is a baby tooth present, it will be removed at the same time. Once the tooth is exposed, the oral surgeon will bond an orthodontic bracket to the exposed tooth. The bracket will have a miniature gold chain attached to it. The oral surgeon will guide the chain back to the orthodontic arch wire where it will be temporarily attached. Sometimes the surgeon will leave the exposed impacted tooth completely uncovered by suturing the gum up high above the tooth or making a window in the gum covering the tooth (on selected cases located on the roof of the mouth). Most of the time, the gum will be returned to its original location and sutured back with only the chain remaining visible as it exits a small hole in the gum.
Shortly after surgery (1-14 days) the patient will return to the orthodontist. A rubber band will be attached to the chain to put a light eruptive pulling force on the impacted tooth. This will begin the process of moving the tooth into its proper place in the dental arch. This is a carefully controlled, slow process that may take up to a full year to complete. Remember, the goal is to erupt the impacted tooth and not to extract it! Once the tooth is moved into the arch in its final position, the gum around it will be evaluated to make sure it is sufficiently strong and healthy to last for a lifetime of chewing and tooth brushing. In some circumstances, especially those where the tooth had to be moved a long distance, there may be some minor “gum surgery” required to add bulk to the gum tissue over the relocated tooth so it remains healthy during normal function. Your dentist or orthodontist will explain this situation to you if it applies to your specific situation.
These basic principals can be adapted to apply to any impacted tooth in the mouth. It is not that uncommon for both of the maxillary cuspids to be impacted. In these cases, the space in the dental arch form will be prepared on both sides at once. When the orthodontist is ready, the surgeon will expose and bracket both teeth in the same visit so the patient only has to heal from surgery once. Because the anterior teeth (incisors and cuspids) and the bicuspid teeth are small and have single roots, they are easier to erupt if they get impacted than the posterior molar teeth. The molar teeth are much bigger teeth and have multiple roots making them more difficult to move. The orthodontic maneuvers needed to manipulate an impacted molar tooth can be more complicated because of their location in the back of the dental arch.
Recent studies have revealed that with early identification of impacted eyeteeth (or any other impacted tooth other than wisdom teeth), treatment should be initiated at a younger age. Once the general dentist or hygienist identifies a potential eruption problem, the patient should be referred to the orthodontist for early evaluation. In some cases the patient will be sent to the oral surgeon before braces are even applied to the teeth. As mentioned earlier, the surgeon will be asked to remove over-retained baby teeth and/or selected adult teeth. He will also remove any extra teeth or growths that are blocking eruption of the developing adult teeth. Finally, he may be asked to simply expose an impacted eyetooth without attaching a bracket and chain to it. In reality, this is an easier surgical procedure to perform than having to expose and bracket the impacted tooth. This will encourage some eruption to occur before the tooth becomes totally impacted (stuck). By the time the patient is at the proper age for the orthodontist to apply braces to the dental arch, the eyetooth will have erupted enough that the orthodontist can bond a bracket to it and move it into place without needing to force its eruption. In the long run, this saves time for the patient and means less time in braces (always a plus for any patient!).
The surgery to expose and bracket an impacted tooth is a very straightforward surgical procedure that is performed in the oral surgeon’s office. For most patients, it is performed with using laughing gas and local anesthesia. In selected cases it will be performed under IV sedation if the patient desires to be asleep, but this is generally not necessary for this procedure. The procedure is generally scheduled for 60 minutes if one tooth is being exposed and bracketed and 90 minutes if both sides require treatment. If the procedure only requires exposing the tooth with no bracketing, the time required will be shortened by about one half. These issues will be discussed in detail at your preoperative consultation with your doctor. You can also refer to Preoperative Instructions under Surgical Instructions on this website for a review of any details.
You can expect a limited amount of bleeding from the surgical sites after surgery. Although there will be some discomfort after surgery at the surgical sites, most patients find Tylenol or Advil to be more than adequate to manage any pain they may have. Within two to three days after surgery there is usually little need for any medication at all. There may be some swelling from holding the lip up to visualize the surgical site; it can be minimized by applying ice packs to the lip for the afternoon after surgery. Bruising is not a common finding at all after these cases. A soft, bland diet is recommended at first, but you may resume your normal diet as soon as you feel comfortable chewing. It is advised that you avoid sharp food items like crackers and chips as they will irritate the surgical site if they jab the wound during initial healing. Your doctor will see you seven to ten days after surgery to evaluate the healing process and make sure you are maintaining good oral hygiene. You should plan to see your orthodontist within 1-14 days to activate the eruption process by applying the proper rubber band to the chain on your tooth. As always your doctor is available at the office or can be beeped after hours if any problems should arise after surgery. Simply call Bay Area Oral & Facial Surgery at 361-814-3223 if you have any questions.
The Oral and Facial Surgeon performs the proper treatment of facial injuries. Dr. Teenier is well versed in emergency care, acute treatment, and long-term reconstruction and rehabilitation, – not just for physical reasons but emotional as well. Oral and Maxillofacial Surgeons are trained, skilled and uniquely qualified to manage and treat facial trauma, broken facial bones and severe cuts/. Injuries to the face, by their very nature, impart a high degree of emotional, as well as physical trauma to patients. The science and art of treating these injuries requires special training involving a “hands on” experience and an understanding of how the treatment provided will influence the patient’s long term function and appearance.
Dr Teenier meets and exceeds these modern standards. He is trained, skilled, and uniquely qualified to manage and treat facial trauma. He is on staff at local hospitals and delivers emergency room coverage for facial injuries, which include the following conditions:
There are a number of possible causes of facial trauma such as motor vehicle accidents, accidental falls, sports injuries, interpersonal violence, and work-related injuries. Types of facial injuries can range from injuries of teeth to extremely severe injuries of the skin and bones of the face. Typically, facial injuries are classified as either soft tissue injuries (skin and gums), bone injuries (fractures), or injuries to special regions (such as the eyes, facial nerves or the salivary glands).
When soft tissue injuries such as lacerations occur on the face, they are repaired by suturing or use of special skin glue. In addition to the obvious concern of providing a repair that yields the best cosmetic result possible, care is taken to inspect for and treat injuries to structures such as facial nerves, salivary glands, and salivary/tear ducts (or outflow channels for saliva and tears). Dr. Teenier is a well-trained Oral and Facial Surgeon and is proficient at diagnosing and treating all types of facial lacerations.
Fractures of the bones of the face are treated in a manner similar to the fractures in other parts of the body. The specific form of treatment is determined by various factors, which include the location of the fracture, the severity of the fracture, the age, and general health of the patient. When an arm or a leg is fractured, a cast is often applied to stabilize the bone to allow for proper healing. Since a cast cannot be placed on the face, other means have been developed to stabilize facial fractures.
One of these options involves wiring the jaws together for certain fractures of the upper and/or lower jaw. Certain other types of fractures of the jaw are best treated and stabilized by the surgical placement of small plates and screws at the involved site. This technique of treatment can often allow for healing and obviates the necessity of having the jaws wired together. This technique is called "rigid fixation" of a fracture. The relatively recent development and use of rigid fixation has profoundly improved the recovery period for many patients, allowing them to return to normal function more quickly.
The treatment of facial fractures should be accomplished in a thorough and predictable manner. More importantly, the patient's facial appearance should be minimally affected. An attempt at accessing the facial bones through the fewest incisions necessary is always made. At the same time, the incisions that become necessary, are designed to be small and, whenever possible, are placed so that the resultant scar is hidden.
Isolated injuries to teeth are quite common and may require the expertise of various dental specialists. Oral surgeons usually are involved in treating fractures in the supporting bone or in replanting teeth that have been displaced or knocked out. These types of injuries are treated by one of a number of forms of splinting (stabilizing by wiring or bonding teeth together). If a tooth is knocked out, it should be placed in salt water or milk. The sooner the tooth is re-inserted into the dental socket, the better chance it will survive. Therefore, the patient should see a dentist or oral surgeon as soon as possible. Never attempt to wipe the tooth off, since remnants of the ligament that hold the tooth in the jaw are attached and are vital to the success of replanting the tooth. Other dental specialists may be called upon such as endodontists, who may be asked to perform root canal therapy, and/or restorative dentists who may need to repair or rebuild fractured teeth. In the event that injured teeth cannot be saved or repaired, dental implants are often now utilized as replacements for missing teeth.
The proper treatment of facial injuries is in the realm of Oral and Maxillofacial Surgery specialists who are well versed in emergency care, acute treatment, long-term reconstruction, and rehabilitation of the patient.
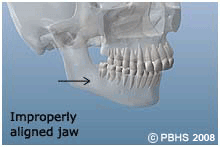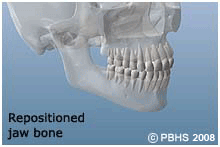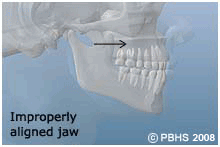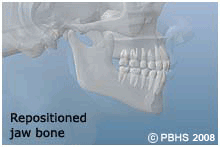
Orthognathic surgery is needed when jaws don't meet correctly and/or teeth don't seem to fit with jaws. Teeth are straightened with orthodontics and corrective jaw surgery repositions a misaligned jaw. This not only improves facial appearance, but also ensures that teeth meet correctly and function properly.
People who can benefit from orthognathic surgery include those with an improper bite or jaws that are positioned incorrectly. Jaw growth is a gradual process and in some instances, the upper and lower jaws may grow at different rates. The result can be a host of problems that can affect chewing function, speech, long-term oral health, jaw joint and problems and appearance. Injury to the jaw and birth defects, congenital malformations/syndromes, can also affect jaw alignment. Orthodontics alone can correct bite problems when only the teeth are involved. Orthognathic surgery may be required for the jaws when repositioning in necessary.
Any of these symptoms can exist at birth, be acquired after birth as a result of hereditary or environmental influences, or as a result of trauma to the face. Before any treatment begins, a consultation will be held to perform a complete examination with x-rays. During the pre-treatment consultation process, feel free to ask any questions that you have regarding your treatment. When you are fully informed about the aspects of your care, you and your dental team can make the decision to proceed with treatment together.
Dr. Teenier uses modern computer techniques and three-dimensional models to show you exactly how your surgery will be approached. Using comprehensive facial x-rays and computer video imaging, we can show you how your bite will be improved and even give you an idea of how you'll look after surgery. This helps you understand the surgical process and the extent of the treatment prescribed. Our goal is to help you understand the benefits of orthognathic surgery.
If you are a candidate for corrective jaw surgery, Dr. Teenier will work closely with your orthodontist during your treatment. The actual surgery can move your teeth and jaws into a new position that results in a more attractive, functional, and healthy dental-facial relationship.
The inside of the mouth is normally lined with a special type of skin (mucosa) that is smooth and coral pink in color. Any alteration in this appearance could be a warning sign for a pathological process. The most serious of these is oral cancer. The following can be signs at the beginning of a pathologic process or cancerous growth:
These changes can be detected on the lips, cheeks, palate, and gum tissue around the teeth, tongue, face and/or neck. Pain does not always occur with pathology, and curiously, is not often associated with oral cancer. However, any patient with facial and/or oral pain without an obvious cause or reason may also be at risk for oral cancer.
We would recommend performing an oral cancer self-examination monthly and remember that your mouth is one of your body's most important warning systems. Do not ignore suspicious lumps or sores. Please contact us so we may help.
Dr. Teenier performs a wide range of Head and Neck Surgeries for being and malignant (cancerous and non cancerous tumors) ranging from the skin to the oral cavity and the head and neck area. He has an intense expertise and interest in this area, and is fellowship trained in Head and Neck Surgery . Everyone’s situation is complex and unique please contact our office for a complete examination and consultation with the Doctor concerning your issues.
What does the term distraction osteogenesis mean? Simply stated, distraction osteogenesis means the slow movement apart (distraction) of two bony segments in a manner such that new bone is allowed to fill in the gap created by the separating bony segments.
Distraction osteogenesis (DO) is a relatively new method of treatment for selected deformities and defects of the oral and facial skeleton. It was first used in 1903. In the 1950s, the Russian orthopedic surgeon, Dr. Gabriel Ilizarov slowly perfected the surgical and postoperative management of distraction osteogenesis treatment to correct deformities and repair defects of the arms and legs. His work went mostly unnoticed until he presented to the Western Medical Society in the mid-1960s.
Distraction osteogenesis was initially used to treat defects of the oral and facial region in 1990. Since then, the surgical and technological advances made in the field of distraction osteogenesis have provided the Oral and Maxillofacial Surgeons with a safe and predictable method to treat selected deformities of the oral and facial skeleton.
Dr. Teenier uses distraction osteogenesis occasionally to treat selected deformities and defects of the oral and facial skeleton. If you have questions about distraction osteogenesis, please call our office and schedule an appointment with Dr. Teenier.
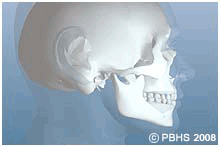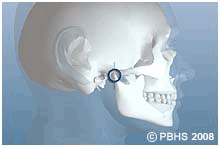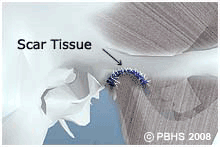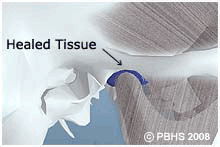
TMJ (temporomandibular joint) disorders are a family of problems related to your complex jaw joint. If you have had symptoms like pain or a "clicking" sound, you'll be glad to know that these problems are more easily diagnosed and treated than they were in the past. These symptoms occur when the joints of the jaw and the chewing muscles (muscles of mastication) do not work together correctly. TMJ stands for temporomandibular joint, which is the name for each joint (right and left) that connects your jaw to your skull. Since some types of TMJ problems can lead to more serious conditions, early detection and treatment are important.
No one treatment can resolve TMJ disorders completely and treatment takes time to become effective. Dr. Teenier can help you have a healthier and more comfortable jaw.
TMJ disorders develop for many reasons. You might clench or grind your teeth, tightening your jaw muscles and stressing your TM joint. You may have a damaged jaw joint due to injury or disease. Injuries and arthritis can damage the joint directly or stretch or tear the muscle ligaments. As a result, the disk, which is made of cartilage and functions as the “cushion” of the jaw joint, can slip out of position. Whatever the cause, the results may include a misaligned bite, pain, clicking, or grating noise when you open your mouth or trouble opening your mouth wide.
The more times you answered "yes", the more likely it is that you have a TMJ disorder. Understanding TMJ disorders will also help you understand how they are treated.
There are various treatment options that Dr. Teenier can utilize to improve the harmony and function of your jaw. Once an evaluation confirms a diagnosis of TMJ disorder, Dr. Teenier will determine the proper course of treatment. It is important to note that treatment always works best with a team approach of self-care joined with professional care.
The initial goals are to relieve the muscle spasm and joint pain. This is usually accomplished with a pain reliever, anti-inflammatory, or muscle relaxant. Steroids can be injected directly into the joints to reduce pain and inflammation. Self-care treatments can often be effective as well and include:
Stress management techniques such as biofeedback or physical therapy may also be recommended, as well as a temporary, clear plastic appliance known as a splint. A splint (or nightguard) fits over your top or bottom teeth and helps keep your teeth apart, thereby relaxing the muscles and reducing pain. There are different types of appliances used for different purposes. A nightguard helps you stop clenching or grinding your teeth and reduces muscle tension at night and helps to protect the cartilage and joint surfaces. An anterior positioning appliance moves your jaw forward, relives pressure on parts of your jaw and aids in disk repositioning. It may be worn 24 hours/day to help your jaw heal. An orthotic stabilization appliance is worn 24 hours/day or just at night to move your jaw into proper position. Appliances also help to protect from tooth wear.
If your TMJ disorder has caused problems with how your teeth fit together, you may need treatment such as bite adjustment (equilibration), orthodontics with or without jaw reconstruction, or restorative dental work. Surgical options such as arthroscopy and open joint repair restructuring are sometimes needed, but are reserved for severe cases. Dr. Teenier does not consider TMJ surgery unless the jaw can’t open, is dislocated and nonreducible, has severe degeneration, or the patient has undergone appliance treatment unsuccessfully.
People with obstructive sleep apnea (OSA) have disrupted sleep and low blood oxygen levels. When obstructive sleep apnea occurs, the tongue is sucked against the back of the throat. This blocks the upper airway and airflow stops. When the oxygen level in the brain becomes low enough, the sleeper partially awakens, the obstruction in the throat clears, and the flow of air starts again, usually with a loud gasp.
Repeated cycles of decreased oxygenation lead to very serious cardiovascular problems. Additionally, these individuals suffer from excessive daytime sleepiness, depression, and loss of concentration.
Some patients have obstructions that are less severe called Upper Airway Resistance Syndrome (UARS). In either case, the individuals suffer many of the same symptoms.
The first step in treatment resides in recognition of the symptoms and seeking appropriate consultation. Oral and Maxillofacial Surgeons offer consultation and treatment options.
In addition to a detailed history, the doctors will assess the anatomic relationships in the maxillofacial region. With cephalometic (skull x-ray) analysis, the doctors can ascertain the level of obstruction. Sometimes a naso-pharyngeal exam is done with a flexible fiber-optic camera. To confirm the amount of cardiovascular compromise and decreased oxygenation levels, a sleep study may be recommended to monitor an individual overnight.
There are several treatment options available. An initial treatment may consist of using a nasal CPAP machine that delivers pressurized oxygen through a nasal mask to limit obstruction at night. One of the surgical options is an uvulo-palato-pharyngo-plasty (UPPP), which is performed in the back of the soft palate and throat. A similar procedure is sometimes done with the assistance of a laser and is called a laser assisted uvulo-palato-plasty (LAUPP). In other cases, a radio-frequency probe is utilized to tighten the soft palate. These procedures usually performed under light IV sedation in the office.
In more complex cases, the bones of the upper and lower jaw may be repositioned to increase the size of the airway (orthognathic surgery). This procedure is done in the hospital under general anesthesia and requires a one to two day overnight stay in the hospital.
OSA is a very serious condition that needs careful attention and treatment. Most major medical plans offer coverage for diagnosis and treatment.
During early pregnancy, separate areas of the face develop individually and then join together, including the left and right sides of the roof of the mouth and lips. However, if some parts do not join properly, sections don’t meet and the result is a cleft. If the separation occurs in the upper lip, the child is said to have a cleft lip.
A completely formed lip is important not only for a normal facial appearance but also for sucking and to form certain sounds made during speech. A cleft lip is a condition that creates an opening in the upper lip between the mouth and nose. It looks as though there is a split in the lip. It can range from a slight notch in the colored portion of the lip to complete separation in one or both sides of the lip extending up and into the nose. A cleft on one side is called a unilateral cleft. If a cleft occurs on both sides, it is called a bilateral cleft.
A cleft in the gum may occur in association with a cleft lip. This may range from a small notch in the gum to a complete division of the gum into separate parts. A similar defect in the roof of the mouth is called a cleft palate.
The palate is the roof of your mouth. It is made of bone and muscle and is covered by a thin, wet skin that forms the red covering inside the mouth. You can feel your own palate by running your tongue over the top of your mouth. Its purpose is to separate your nose from your mouth. The palate has an extremely important role during speech because when you talk, it prevents air from blowing out of your nose instead of your mouth. The palate is also very important when eating. It prevents food and liquids from going up into the nose.
As in cleft lip, a cleft palate occurs in early pregnancy when separate areas of the face have developed individually do not join together properly. A cleft palate occurs when there is an opening in the roof of the mouth. The back of the palate is called the soft palate and the front is known as the hard palate. A cleft palate can range from just an opening at the back of the soft palate to a nearly complete separation of the roof of the mouth (soft and hard palate).
Sometimes a baby with a cleft palate may have a small chin and a few babies with this combination may have difficulties with breathing easily. This condition may be called Pierre Robin sequence.
Since the lip and palate develop separately, it is possible for a child to be born with a cleft lip, palate or both. Cleft defects occur in about one out of every 800 babies.
Children born with either or both of these conditions usually need the skills of several professionals to manage the problems associated with the defect such as feeding, speech, hearing and psychological development. In most cases, surgery is recommended. When surgery is done by an experienced, qualified Oral and Maxillofacial Surgeon such as Dr. Teenier, the results can be quite positive.
Cleft lip surgery is usually performed when the child is about ten years old. The goal of surgery is to close the separation, restore muscle function, and provide a normal shape to the mouth. The nostril deformity may be improved as a result of the procedure or may require a subsequent surgery.
A cleft palate is initially treated with surgery safely when the child is between 7 to 18 months old. This depends upon the individual child and his/her own situation. For example, if the child has other associated health problems, it is likely that the surgery will be delayed.
The major goals of surgery are to:
There are many different techniques that surgeons will use to accomplish these goals. The choice of techniques may vary between surgeons and should be discussed between the parents and the surgeon prior to surgery.
The cleft hard palate is generally repaired between the ages of 8 and 12 when the cuspid teeth begin to develop. The procedure involves placement of bone from the hip into the bony defect, and closure of the communication from the nose to the gum tissue in three layers. It may also be performed in teenagers and adults as an individual procedure or combined with corrective jaw surgery.
After the palate has been fixed, children will immediately have an easier time in swallowing food and liquids. However, in about one out of every five children following cleft palate repair, a portion of the repair will split, causing a new hole to form between the nose and mouth. If small, this hole may result in only an occasional minor leakage of fluids into the nose. If large however, it can cause significant eating problems, and most importantly, can even affect how the child speaks. This hole is referred to as a "fistula," and may need further surgery to correct.
Dr. Teenier performs rhinoplasty in order to reshape the nose. Appearance can be improved for those people who are dissatisfied with the shape and size of their nose. Nasal reconstruction was one of the first cosmetic procedures ever developed and is among those most frequently performed today. Rhinoplasty is a surgical procedure in which deformities of the nose are corrected by removing, rearranging, or reshaping bone or cartilage.
Reasons include reducing the size of the nose, removal of bumps as well as improving the angle of a nose. Conditions may be natural or due to external trauma to the face. This operation will also help patients who have difficulty breathing. The operation can be performed on all age groups, including teens and the elderly.
A medical history along with a careful examination is conducted in order to evaluate your general health. We will discuss with you the way your nose can look in relation to your other facial features. Digital photographs and computer imaging allow Dr. Teenier to evaluate the appropriate procedure to achieve the desired results. Preoperative instructions may include eliminating certain drugs that contain aspirin to minimize the possibility of excess bleeding. Antibiotics may be prescribed before surgery to prevent infection.
Surgery is usually performed under IV sedation, which is both extremely comfortable and results in less swelling and bruising than general anesthesia. In most cases involving a reduction in shape or size of the nose, angle, or removal of a hump, the skin of the nose is separated from the underlying skeleton of bone and cartilage. The bone and cartilage are then reshaped and the skin redraped over the surface. Patients who have a deviated septum may benefit by correction of this problem. The incisions are placed inside the nose, unless the surgeon uses an open approach, in which case the incisions are made across the columella (the tissue between the nostrils). In cases where the nostrils flare, the surgeon may make an incision at the junction between the nose and the skin of the upper lip to narrow the flared appearance. It is not unusual to combine rhinoplasty with chin augmentation to improve the profile.
The recovery takes one to two weeks. Most people resume their normal activities within a week or two. Following surgery, a lightweight splint is applied to maintain the new shape of the nose. The splint is removed within a week. Nasal splints may be inserted at the time of surgery to protect the septum. These are removed within a week. There is always some stuffiness of the nose, especially when work has been done on the nasal septum.
Pain is minimal and is controlled with medications. Bruising occurs around the eyes and begins to fade within a few days. Discoloration usually disappears in two weeks.
Dr. Teenier performs brow and forehead lifts to raise eyebrows and reduce ridges and furrows on the forehead, creating a smoother, more youthful appearance. This procedure can be performed in conjunction with other surgeries.
An incision is generally made across the top of the head from the front of one ear to the front of the other ear. The forehead and brows are elevated and excess skin is removed. The flap is then sutured. Newer techniques now allow us to perform forehead lifting through small incisions in the scalp by using an endoscope and specialized instruments. This accelerates the healing process.
Antibiotics may be prescribed for several days following surgery. Sutures are generally removed within one week. Swelling and some bruising may occur which should subside within a few weeks. Our doctors will prescribe ice compresses and eye exercises to reduce swelling and regain mobility. Women will be allowed to use eye cosmetics two weeks after surgery. You can proceed with your normal daily activities within one to two weeks. A final evaluation may occur within several months from the initial surgical procedure.
Many factors cause the skin to wrinkle and sag (i.e., exposure to the sun, genetics as well as the natural aging process). Children and young adults have smooth, round faces due to fatty tissue that is evenly distributed throughout the contours of the face. As you age, the skin sags and fits more loosely. These folds become prominent, especially around the chin, the jaw line, and along the neck.
Dr. Teenier performs rhytidectomies, or facelifts, to enhance your appearance and correct these conditions. A facelift involves tightening of the facial and neck muscles as well as the removal of any excess skin. The procedure is often performed in conjunction with additional cosmetic surgeries such as blepharoplasty (eyelid surgery), forehead lift, chin augmentation, liposuction, and/or rhinoplasty (nasal surgery). These procedures can be performed any time after signs of aging appear in order to attain a more youthful appearance.
We will evaluate your medical history in order to determine your overall health. Dr. Teenier will discuss with you how your face can look and what you can expect from surgery. Our objective is to create a natural appearance that is pleasing to you. Photographs and computer imaging are performed to determine the amount of improvement after surgery.
We will provide you with preoperative instructions that may include the elimination of specific drugs containing aspirin several weeks before surgery to minimize excess bleeding. Antibiotics may also be prescribed to prevent infection. You may be instructed to shampoo your hair the night before surgery. A small amount of hair may be shaved around your ears and temples.
A rhytidectomy can be performed under IV sedation or general anesthesia in our state-of-the-art surgical facility. These options will be discussed in detail with you. Premedication is administered for relaxation. Incisions are made inside the hairline at the temple, running in front of the ear then around the earlobe and behind the ear, ending in the hair of the scalp. The loose skin is separated from underlying tissue and is pulled up and back. Excess skin is removed. Sagging muscles and connective tissues are tightened. In some cases, fatty deposits are removed from beneath the chin and neck. Small sutures are used to close the incisions. The procedure may take up to five hours depending on whether any other procedures are performed at the same time.
It is recommended that you stay one night in the recovery care center to receive specialized care from the nursing staff. Bandages are applied to the area of surgery and are removed within a few days. Pain is moderate and controlled with oral medications. Your sutures are removed within the first five to ten days. In order to minimize scarring, the doctor may remove the sutures in stages. Scarring fades quickly. Swelling and discoloration decrease within two weeks. Tightness in your face will be present for several weeks and there may be slight changes in your hair pattern around the incision.
It is recommended that you avoid the sun for several weeks after surgery. Healing is gradual so you will not notice final results for up to six months. Improvement varies, depending on the your initial condition. In most cases, a single procedure achieves the desired results. Most patients who have had facelifts are pleased with their new, more youthful appearance.
As we all know, the eyes are a prominent facial feature. Although the eyes are expressionless structures, the surrounding skin conveys emotion. The tissue, muscle, fat, hair, and lashes all contribute to the wide array of expressions. Unfortunately, wrinkles and deep lines as well as puffiness under the lids develop as you age. In addition, exposure to the sun as well as hereditary factors contribute to the aging process, all resulting in changes of expression. In many cases, people may look fatigued, worn out, and older than their true age. Beyond possible visual impairment, these changes in your appearance can cause stress and anxiety.
Dr. Teenier is trained in several surgical procedures, such as blepharoplasty, forehead lift, and brow lift in order to eliminate the majority of these problems.
We can perform blepharoplasty to correct sagging eyelids, bags or pouches beneath the eyes, as well as excess folds around the eyes. This surgical procedure involves the removal of excess skin and fat on upper and lower eyelids and is often performed in conjunction with other surgical procedures including facelifts, eyebrow, and forehead lifts. Blepharoplasty can be done under general anesthesia (with you asleep) or under IV sedation. Both are very comfortable options. Premedication is utilized prior to surgery to decrease swelling after the operation.
Dr. Teenier will trace the natural lines and creases of your face and make incredibly fine incisions from the inner to the outer edge of the eyelid. Surgery on the upper eyelid is performed first with the incision made in the fold of the lid. The incision is made below the eyelash on the lower eyelid. Any excess fat and skin are removed from the underlying compartments. The amount of fat excised is determined by the degree of protrusion of fat when pressure is applied to the area. Small sutures are used to close the incision and special ointments and dressings may be applied. The surgery can take up to two hours. In certain cases, lower eyelid incisions are made inside the lid. Laser may be used at the same time to reduce wrinkles.
Initially, drying of the eyes can occur after blepharoplasty. This condition can be alleviated with medication. In addition, you may be sensitive to bright light and wind for a period of time. Numbness and itching may also occur during the healing process. A final evaluation may occur within several months from the initial surgical procedure.
Facial liposuction is a very common and popular procedure. It is designed for the permanent removal of fatty tissue from your cheeks, chin, and neck. It is an elective procedure that allows the surgeon to remove undesirable, subcutaneous fat in specific areas that do not respond to diet and exercise.
Patients with good skin tone who have fatty deposits receive the best results from facial liposuction. It is not a treatment for obesity. If weight gain occurs following liposuction, the fat will be deposited in areas that have not been treated. The procedure can be repeated, if necessary. To maintain the safety of the procedure, there is a limit on how much can be done at one time. A variety of factors can affect the results: physical condition, genetic makeup, diet, exercise, smoking, alcohol intake, and skin elasticity.
Facial liposuction is performed under general anesthesia on an outpatient basis in a hospital or surgical center. The surgeon makes small (less than 1/2 inch), discreet incisions in the face or neck. A cannula is inserted in a small incision and attached to a suction machine. The procedure may take an hour or more.
The results of liposuction are permanent. If you were to gain a large amount of weight, you might note rippling in the treated areas, depending on your skin elasticity.Following liposuction, the scar will go through a maturation process. During the first eight to twelve weeks, they may be red and possibly raised. The scars will mature over six to twelve months and become pale, flat, and soft. You may experience numbness, burning, and/or tingling around the incision site. These symptoms are almost always temporary. Please let us know if you are prone to keloid scars.
In cases of protruding or over-developed ears, the procedure of otoplasty may be an option. Otoplasty is commonly referred to as "pinning back" of the ears. It is available for children once their ears have stopped developing around the age of six. Over-developed ears can be the cause of psychological stress and trauma and should be treated at a young age before it becomes a serious issue. Dr. Teenier is trained in several surgical procedures that eliminate the majority of the problems related to protruding ears.
The procedure can be performed under IV sedation or general anesthesia and the doctor will discuss this option with you. Dr. Teenier has the option of either folding the cartilage located on the back of the ear or removing excess cartilage. Sutures are placed and bandages applied to speed the healing process. The procedure typically takes only a few hours.
After the operation patients should expect bruising around the area that fades in two to three weeks. Pain associated with operation is minimal and can be easily treated with oral medication. The bandages are only needed for a few days and should be replaced with a lighter dressing. Refraining from sleeping on the ears is required and patients are advised to use a very soft pillow. Showering and shampooing may begin after a few days. Expect two to three days of recovery before normal activities can be performed. Consult with Dr. Teenier before attempting any athletic or precarious activities that may affect the healing process.
BOTOX® Cosmetic treatment is a revolutionary approach to reversing the affects of facial wrinkles. Crow’s feet, worry lines, and laugh lines can all be a thing of the past. These are referred to as dynamic wrinkle lines and all are treatable with this procedure. Cosmetic denervation is the process of injecting BOTOX® Cosmetic into the tiny facial muscles that create the wrinkles.
To better understand your overall health, we will evaluate your medical history prior to surgery. In addition, a complete examination of your eyes is made in order to decide the most effective injection sites. All issues and concerns will be discussed.
The areas that will be treated are marked and digital photographs are taken in order to determine the amount of improvement after surgery.
BOTOX® Cosmetic injections are performed without anesthesia because they are virtually painless. Only a very small sting is felt when the injections are made. The effects are not permanent and may need to be repeated two to three times per year to retain the effects. Research has suggested, however, that long-term use of the injections leads to a longer duration of each treatment's effect. Patients over the age of 65 may not experience such dramatic results. BOTOX® Cosmetic is only useful in treating expression lines and cannot be used to repair sagging skin caused by aging.
After the operation patients may experience slight bruising around the area that quickly fades. Normal activities can be performed immediately. Possible side effects are temporary weakness of nearby muscles or in rare cases an eyelid may droop. BOTOX® Cosmetic is completely reversible so any side effect is only a temporary condition. The doctor will explain all risks associated at the time of your consultation.
A chemical peel is helpful for wrinkles, light acne scarring, and irregular pigmentation such as freckles and age spots. Pre-cancerous conditions such as keratoses (thick, rough, reddish growths) also respond well to this procedure.
There are several types of chemical peels: light peels remove superficial wrinkles, medium, and deep peels are for more severe conditions.
After a thoroughly cleansing of the skin, a small applicator is used to apply the chemical solution to an area of the face. Excess solution is removed and the procedure is repeated on other areas.
The amount of improvement varies and depends upon the initial condition of the patient's skin. Significant improvement of damaged skin has been achieved, which can produce dramatic results.
Several methods of anesthesia are available. The method of anesthesia that is chosen for or by a patient depends upon the nature of the surgical procedure and the patient's level of apprehension, difficulty of the procedure and health of the patient. The following table illustrates the choices of anesthesia, a description of the anesthetic technique, and the usual indications for that technique.
Method of Anesthesia |
Description of Technique |
Usual Indications |
| Local Anesthetic | The patient remains totally conscious throughout the procedure. A local anesthetic (e.g. lidocaine) is administered in the area where the surgery is to be performed. Local anesthetic is used in conjunction with the other methods of anesthesia in all oral surgery procedures. | Simple oral surgery procedures such as minor soft tissue procedures such as simple biopsy. |
| Nitrous Oxide Sedation with Local Anesthetic sometimes augmented with a Valium like pill |
A mixture of nitrous oxide (laughing gas) and oxygen is administered through a nasal breathing apparatus. The patient remains conscious in a relaxed condition. Nitrous oxide has a sedative and analgesic (pain- controlling) effect, sometimes augmented with a valium like pill. |
Simple oral surgery procedures to more involved procedures or where the level of patient apprehension is elevated |
| Intravenous Anesthesia Office Based General Anesthesia, or sedation with Local Anesthetic* |
Medications are administered through an intravenous line (I.V.). The patient falls asleep and is unaware of the procedure being performed. Medications most commonly used are Fentanyl, Nubain (opiate), Versed (benzodiazepine), Ketamine, and Diprivan. Supplemental oxygen is delivered through a nasal breathing apparatus and the patient's vital signs are closely monitored. | General anesthesia and/or intravenous anesthesia are available for all types of oral surgery. A patient may choose this option for simple procedures depending on their level of anxiety. Most people having their wisdom teeth removed or having a dental implant placed will choose general anesthesia and/or intravenous sedation, more involved soft tissue operations such as biopsies or cosmetic procedures. General anesthesia and/or intravenous sedation may be necessary if local anesthesia fails to anesthetize the surgical site which often occurs in the presence of infection. |
| Hospital or Surgery Center Based General Anesthesia | A patient is admitted to a hospital or surgery center where anesthesia is administered by an anesthesiologist. | Indicated for patients undergoing extensive procedures such as face and jaw reconstruction, tumor/cancer surgery, sinus surgery and/or cosmetic surgery. Also indicated for patients with serious or several medical conditions such as heart disease or lung disease who require general anesthesia. |
*To administer general anesthesia and/or intravenous sedation in the office, an oral surgeon must have completed at least three months of hospital based anesthesia training. Qualified applicants will then undergo an in office evaluation by a state board appointed examiner. The examiner observes an actual surgical procedure during which general anesthesia is administered to the patient. The examiner also inspects all monitoring devices and emergency equipment and tests the doctor and the surgical staff on anesthesia related emergencies. If the examiner reports successful completion of the evaluation process, the state board will issue the doctor a license to perform general anesthesia and/or intravenous sedation. The license is renewable every two years if the doctor maintains the required amount of continuing education units related to anesthesia.
Again, when it comes to anesthesia, our first priority is the patient's comfort and safety. If you have any concerns regarding the type of anesthesia that will be administered during your oral surgery procedure, please do not hesitate to discuss your concerns with your doctor at the time of your consultation.
Our office offers our patients the option of Intravenous Sedation or Intravenous Anesthesia or to some it has been referred to as "Twilight Sedation" for their treatment. Intravenous Sedation or "twilight sleep" helps you to be comfortable and calm when undergoing procedures. Your treatment can be completed under intravenous sedation. Intravenous sedation or “IV sedation” (twilight sedation) is designed to better enable you to undergo your dental procedures while you are very relaxed; it will enable you to tolerate as well as not remember those procedures that may be very uncomfortable for you. IV sedation will essentially help alleviate the anxiety associated with your treatment. You may not always be asleep, unconscious but you will be comfortable, calm and relaxed, drifting in and out of sleep – a “twilight sleep”.
If you choose the option of intravenous sedation your IV sedation/anesthesia is administered and monitored by Dr. Teenier therefore eliminating the costly expense of having your treatment carried out in an operating room or same day surgical facility.
How is the IV Sedation Administered?
A thin pediatric needle will be introduced into a vein in your arm or hand. The needle will be attached to an intravenous tube through which medication will be given to help you relax and feel comfortable. At times a patient's vein may not be maintainable, in these situations the medications will be administered intramuscularly and the needle retrieved - both scenarios will achieve the same desired level of conscious sedation. Once again some patients may be asleep while others will slip in and out of sleep. Some patients with medical conditions and/or on specific drug regimens may only be lightly sedated and may not sleep at all but be relaxed.
The goal of IV sedation is to use as little medication as possible to get the treatment completed. It is very safe, much safer than oral sedation. With IV sedation a constant “drip” is maintained via the intravenous tube. At any time an antidote can be administered to reverse the effects of the medications if necessary. Along with IV sedation there are also other different “levels” of sedation available to you in our office.
Nitrous Oxide is a sweet smelling, non irritating, colorless gas which you can breathe. Nitrous Oxide has been the primary means of sedation in dentistry for many years. Nitrous oxide is safe; the patient receives 50-70% oxygen with no less than 30% nitrous oxide. Patients are able to breathe on their own and remain in control of all bodily functions. The patient may experience mild amnesia and may fall asleep not remembering all of what happened during their procedure.
Though there are no major contraindications to using nitrous oxide, you may not want to use it if you have emphysema, exotic chest problems, M.S., a cold or other difficulties with breathing. You may want to ask your doctor for a "5 minute trial" to see how you feel with this type of sedation method before proceeding.
In some cases such as phobias, the patient and MD may elect to use a valium like pill prior to any of the above anesthetic techniques. This is decided on a case by case basis. If you do fear treatments at the doctor please discuss this with Dr. Teenier.
Our online videos are presented in order to help you understand more about the oral surgery procedures we perform. Please choose a specific video of your interest.
Having trouble? Please make sure you have version 7 of the Flash browser plugin in order to correctly view this presentation. This software is available as a free download.
The following websites are provided as a resource for our referring doctors. This page contains hyperlinks to World Wide Web sites that are created and maintained by other organizations. We have included these links because we think that our referring doctors may find them of interest. Keep in mind that Bay Area Oral & Facial Surgery does not necessarily endorse the views expressed on these websites. Also, we do not guarantee the accuracy or completeness of any information presented on these sites.
List of International Dental School Website
WebDental - American based dental database
Cambridge University Medical Library
Medical Library University of Manchester
MedicineNet - Content-rich commercial site includes interactive groups, ask-the-doctor feature, medical dictionary, comprehensive drug information, medical news, disease-specific information, and links.
Medscape - Searchable commercial collection of full-text articles from such useful sources as the National Institutes of Health and the Centers for Disease Control and Prevention.
Oncolink - Huge collection of cancer information and links based at the University of Pennsylvania. The best starting place found for cancer information.
ParentsPlace.com - Not health-only, but this commercial site contains many pages of sophisticated, reader friendly information on children's health issues.
Medical Matrix - Physician maintained commercial database of annotated health links. Oriented toward medical professionals, but accessible to an educated lay person. A keyword search gets you to a subject index, from which you navigate to the links you want.
American Journal of Oral and Maxillofacial Surgery
Journal of Cranio-Maxillofacial Surgery
Nature - International weekly journal of science
New England Journal of Medicine
American Academy of Dermatology
American Academy of Implant Dentistry
American Academy of Restorative Dentistry
American Association of Endodontists - national organization representing the specialty of endodontics or root canal treatment.
American Academy of Periodontology - mission is to advance the periodontal health of the public and represent and serve the members of the academy.
American Association of Oral & Maxillofacial Surgeons - find information about Oral and Maxillofacial Surgery including cancer, dental implants, sports safety, jaw surgery, and more.
American Association of Women Dentists - dedicated to enhancing and promoting participation and leadership for women in organized dentistry.
American College of Oral and Maxillofacial Surgeons
American College of Prosthodontics
American Dental Association - ADA Online - access to news, publications, and products and services related to dental health.
American Endodontic Society, Inc. - endorses and teaches the Sargenti or N2 technique of root canal therapy.
American Independent Dentist's Association - dedicated to the survival of the concept of optimal care in dentistry. Working to re-engineer organized dentistry and bring new tools to the education of patients.
American Medical Association - another useful site with links to consumer health information, vast AIDS information center, searchable database of more than 650,000 physicians
American Society for Dental Aesthetics
American Society of Dentist Anesthesiologists
Association of Managed Care Dentists - a non-profit organization dedicated to the education of dentists and related professionals about the emerging managed care delivery systems.
Center for Reconstructive Jaw Surgery
Craniomaxillofacial Surgery Database Membership
Craniomaxillofacial Surgery Related Sites
Crown Council - dental professionals dedicated to continual improvement of their clinical and management skills.
International Association of Dental Research
International Association for Disability and Oral Health - general informational brochure and quarterly newsletter information.
International Association of Dento-Maxillo-Facial Radiology
International Congress of Oral Implantologists (ICOI) - professional organization of dental implantology specialists.
National Association of Dental Laboratories (NADL) - contains news, general and membership information, links, and a forum.
National Association of Dental Plans - NADP representative and recognized resource of the dental HMO/PPO industry with news, meetings, statistics and other resources.
Oral Cancer Information Center - US based web-site
3i (Implant Innovations, Inc.)
Navigable World Map - (the Virtual Tourist)
Doctor's Searchable Guide - to conferences, journals etc
Medscape - a general medical resource - US based
BBC Search Engine - provides access to many other search engines and services
Home | Patient Information | Procedures | Cosmetic Procedures | Instructions | Meet Us | Online Forms | Referring Doctors | Contact Us | Disclaimer | Sitemap
5402 Holly Road, Building 3, Suite 302, Corpus Christi, TX 78411 | Phone: 361-814-3223 Fax: 361-814-0033
Dental Website Design by PBHS 2011©